Talking to Families About Donation
Centers for Medicare & Medicaid Services (CMS) is a federal agency that has laid out regulations to define the collaborative effort between hospitals and OPOs (organ procurement organizations) in the Conditions of Participation.
In the Conditions of Participation, the person designated by the hospital to initiate the donation conversation to the family must be an organ procurement representative.
Judgment cannot be made by the hospital that certain families should not be approached about donation.
Hospitals should support the family with the belief that donation is possible and should take steps to ensure the family is treated with respect and care.
Hospital staff’s perception that a family’s grief, race, ethnicity, religion, or socioeconomic background would prevent donation should never be used as a reason not to approach a family.
All potential donor families must be approached and informed of their donation rights and give a decision to donate or decline.
When is the best time for donation conversation?
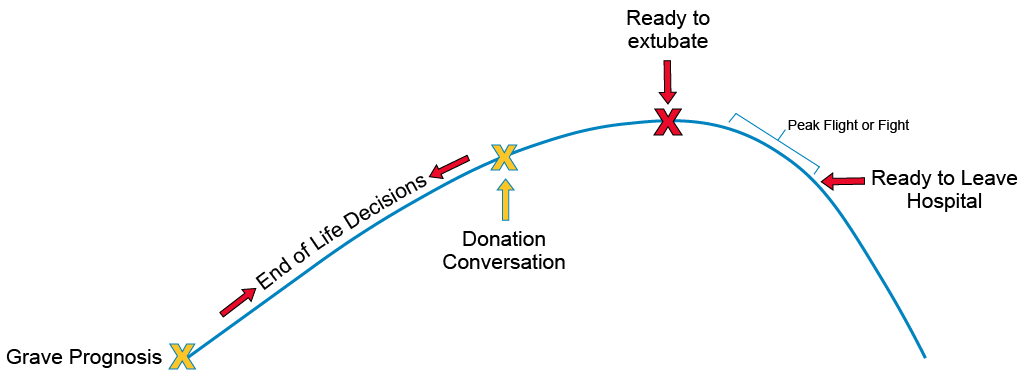
Best practice shows that the best time for the coordinator to speak to families about donation is when families are thinking about what end of life decisions could be or are.
Soft Cues that you may notice
SOFT CUES:
Indicators that identify the family may be ready for interaction with LifeShare
Indicators that identify the family may be ready for interaction with LifeShare
|
Family is asking:
• What is next? • What happens if everything is stopped? • Can we have additional visitation time to say goodbye? • Family asks for Pastoral support or palliative care. • Funeral arrangements are mentioned. • Financial assistance related to end-of-life planning is discussed. • Questions about comfort care. • How long will it take after he/she is disconnected? • To have a meeting with the care team about the plan of care. |
Family may be saying:
• They would not want to live on a ventilator. • We cannot see him/her like this anymore. • Language about their loved one is in the past tense (I remember when). • Family is telling other family and friends how bad the prognosis is over the phone. • Family is calling other family to visit to say goodbye. • Language related to the possibility of removing life sustaining therapies. • He/She has had a good life: we have had a wonderful marriage; he has been the best day, etc. |
Waiting until there is a time or readiness to extubate is often too late and does not give families a fair opportunity to hear about donation.
Evaluating the best time for families to hear about donation is done between the hospital nurse, physician and LifeShare coordinator. A huddle will always occur to determine family readiness.
Who should approach the family?
Only trained staff from LifeShare should bring up donation to families. Hospital staff are always welcome to join the conversation with the requestor.
Why?
• Hospital staff members who first speak to family members about donation can present a conflict of interest
• The patient may not be eligible to donate leading to further disappointment
• Conversations prior to a LifeShare coordinator prevents detailed questions from being answered appropriately
• The patient could be a registered donor
• Hospital staff members who first speak to family members about donation can present a conflict of interest
• The patient may not be eligible to donate leading to further disappointment
• Conversations prior to a LifeShare coordinator prevents detailed questions from being answered appropriately
• The patient could be a registered donor